
Revised 2023
What can I do to improve my chances of getting pregnant naturally?
Before attempting pregnancy, an individual should make sure one is healthy enough for pregnancy by adopting a healthier lifestyle and taking prenatal vitamins. Regarding all supplements, there is no scientific evidence currently promoting their use in enhancing fertility. If one has a medical or genetic condition (or is at risk for one), one should seek advice from a medical professional before conceiving (becoming pregnant).
What are my chances of conceiving?
While there is no simple way to answer this, the two most key factors influencing the success of conception are the age of the individual and the number of months one and their partner have been trying to become pregnant. Young people with female reproductive anatomy with regular menstrual cycles have a 20 to 37% chance of becoming pregnant within the first 3 months, an 80% chance after one year, and a 90% chance after two years.
How often should a couple have intercourse?
The highest pregnancy rates are seen when partners have intercourse every 1 to 2 days during the fertile window. Surprisingly, lengthy periods of abstinence (not having intercourse) can decrease the quality of sperm. Infrequent intercourse may decrease the chance that intercourse will happen around the time of ovulation.
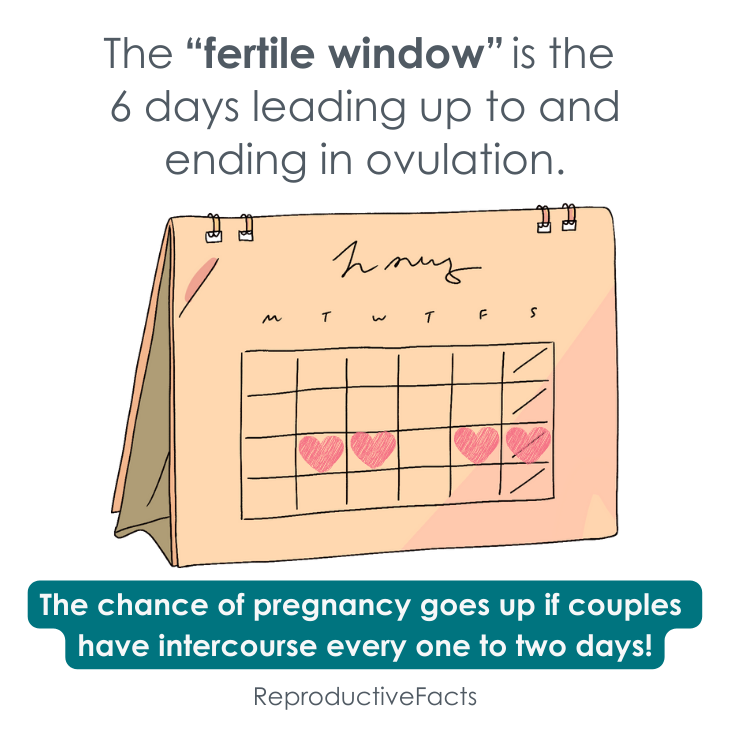
What is the fertile window?
The fertile window is the time in a cycle when pregnancy can occur. It is usually the 6 days just before the day of ovulation. Ovulation occurs around 14 days before the next menstrual period, so an individual with a 28-day cycle will ovulate around cycle day 14 (that is, 14 days after the start of their last menstrual period). That means that pregnancy is most likely to happen if intercourse occurs within the 6 days right before the day of ovulation.
How do I know when I am ovulating?
Because the fertile window is set by the day of ovulation, it is important to know when an individual is ovulating. There are several methods of determining ovulation. Cervical mucus and vaginal secretions start to increase 5 to 6 days prior to ovulation and peak 2 to 3 days before ovulation. These changes can be monitored to identify the fertile window in many individuals and can even be tracked using smartphone applications. Additionally, there are modern applications specifically designed for tracking ovulation, leveraging current technology to provide accurate and user-friendly monitoring. Urinary ovulation predictor kits can also be used to detect the rise in luteinizing hormone (LH) that happens just before ovulation. LH is the primary trigger that results in the eggs being released from the ovary (see ASRM fact sheet titled “Am I ovulating?”).
Are there (intercourse) practices that can improve our chances of conceiving?
Sperm ejaculated or released into the vagina reach the fallopian tubes within minutes regardless of position during intercourse. There is no evidence that sexual position, orgasm, or prolonged rest after intercourse increases the chance of conception. Some lubricants (Astroglide®, KY® Jelly, KY® TouchTM, saliva and olive oil) used during intercourse may decrease sperm motility (movement) or survival. This should be avoided if possible. Others (Pre- Seed®, mineral oil or canola oil) have no such effect and can be used as needed.
Does diet affect fertility?
Smoking, heavy alcohol consumption (> 2 drinks per day), heavy caffeine consumption, and the use of recreational drugs such as marijuana have all been associated with reduced fertility. Therefore, individuals considering pregnancy should reduce alcohol and caffeine use and avoid smoking and all recreational drugs while trying to conceive.
Are there reasons to see a healthcare professional sooner rather than later?
Some individuals or couples have a health history that warrants consulting a healthcare professional either before or early in the process of trying to get pregnant. These warrants include:
 Menstrual and Ovulatory Health
Menstrual and Ovulatory Health
- Irregular or no menstrual periods
- Negative luteinizing hormone tests for ovulation
Sexual Health History
- History of sexually transmitted infection
Pelvic and Abdominal Health
- Prior pelvic or abdominal surgery for any reason
Previous Infertility History
- Prior history of infertility
Partner’s Reproductive Health
- Known problems with the testicles or genitals
- Hypospadias (opening of the urethra not in the end of the penis)
- Sexually transmitted infection
- Problems with ejaculation
- Prior history of infertility
Fact Sheets/Booklets
View more fact sheets and booklets written by the ASRM Patient Education Committee.
Menopausal Transition (Perimenopause): What Is It?
The menopausal transition (perimenopause) is the period that links a woman’s reproductive (childbearing) years and menopause.
Osteoporosis
Osteoporosis and osteopenia are conditions of having low bone mass (density).
Hyperprolactinemia (High Prolactin Levels)
Prolactin is a hormone produced by your pituitary gland which sits at the bottom of the brain.Infertility
Find a Health Professional












